This post marks the start of a short series of posts connected to the subject of my PhD dissertation – vaccines and vaccination policy. I will touch on several disparate aspects of the issues. In this first installment, I will have a look at vaccines and infant mortality – and as it happens, dramatically turn the table on some claims from anti-vaccination activists. Enjoy!
To the extent that vaccine skeptics (actually, let’s just go with anti-vaxxers) deal with real data rather than gut feeling or common tropes about naturalness, toxins, and the like, they tend to do so highly (to say the least) selectively and with a characteristic disregard for normal scientific practice and rules of causal inference. This includes, but is not limited to, two main fundamental errors, namely the post hoc ergo propter hoc fallacy (something happened after, therefore because of, an event, which pertains to claims based on adverse event reporting), and the classic error of confusing correlation for causation.
In this post I will address the second. I will refrain from restating what the fallacy is (I’ve written about it before here). Instead, I will try to wrestle the weapon that this logical fallacy is out of the hands of the anti-vaxxers and show what would happen if we looked at some real data! Bear with me.
Here is an example of when an anti-vaxx argument (for reasons of poor editorial attention, one is forced to conclude) actually made it into the scientific literature. The paper finds that countries with more recommended childhood vaccines have higher infant mortality. Fine. Except this really says nothing about what effects vaccines have on infant mortality. Implying anything about any such connection commits the crucial error of confusing correlation with causation. (Steven Novella has written at length about this paper already – do read!)
The question is – what could we accomplish if we allowed ourselves the same luxury, and refined this type of analysis quite a bit? One of the many fundamental errors in this paper is assuming that the number of recommended vaccines has anything to do with how many vaccines are actually taken – that is, population uptake. Considering that such data is easily available, one might wonder why such an analysis didn’t make it into the paper (given the analysis below, the answer might seem obvious… but let’s not be facetious). Let’s give it a try!
The WHO provides fairly detailed datasets over the shares of newborns that are vaccinated in each country every year. They also have data on relevant measures such as infant mortality and life expectancy – also per country. Interesting! If there was a causal connection in accordance with the paper described above, and we allowed ourselves to confuse correlation with causation (as the authors do), we would have to observe higher infant mortality in countries with higher vaccination uptake. Let’s create a variable that summarizes the average uptake of measles, diphtheria, pertussis and tetanus vaccinations among infants. Here’s how it correlates with infant mortality, for the year 2010:
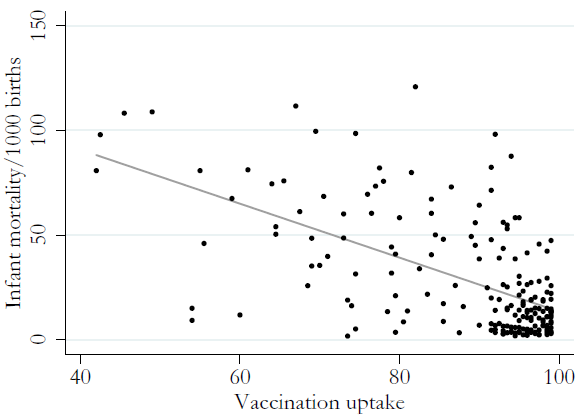
Oops! When looking at actual uptake rates, there is a strong negative correlation: the more infants are vaccinated, the lower the infant mortality rate – and the average differences are stunning.
Now, someone – perhaps even an anti-vaxxer – might say that there is obvious confounding here. Yes, there is, and as it happens, that’s precisely my methodological point! Rich countries can afford more vaccines. And rich countries can also afford other things, like basic sanitation and proper nutrition and clean water and such. Great, now we’re getting somewhere!
In fact, let’s clean up all this variation from a number of possible other explanations: national wealth (logged to account for the diminishing marginal effects of wealth), access to clean water, nutritional status (measured as average calorie deficit), access to health care (measured as number of hospital beds per capita) and access to proper sanitation. We’ll do that in a full dataset spanning most countries in the world for the years 1980-2010, and we’ll do it with good old-fashioned multiple OLS, with fixed effects for both countries and years, and clustered standard errors at the country level to make sure we’re not overestimating the statistical significance of the correlations. The table below shows a number of models with infant mortality rate as the dependent variable (and an unfortunate amount of listwise deletions). All data are from the QoG database.
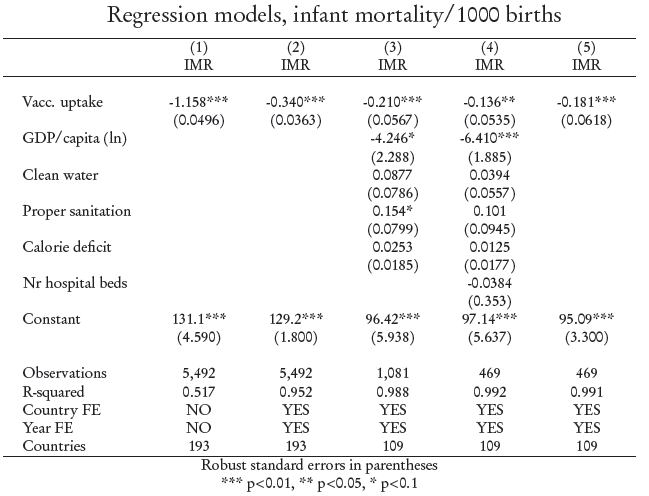
For those who may not be used to interpreting regression tables, the most conservative estimate of the correlation, when all of the above mentioned other explanatory factors are controlled for, is a predicted reduction in infant mortality by more than ten deaths per 1000 births if a country with very low vaccination coverage were to vaccinate most of its infants. How big of a difference is that? It’s the difference between the Gaza strip and the United states.
Does this say that higher vaccination uptake definitely causes lower infant mortality? No – we should generally have higher standards of evidence than this. Despite controlling for a number of confounders and taking time trends into account (and more), this is not a robust causal estimate, and it may be both weaker or stronger in reality. My point is that this estimate, if anything, is at the very least vastly more methodologically credible than any of the ones I’ve seen (even published) from anti-vaxxers – and I threw this together in half an hour with easily available data.
So what’s the lesson then? We know that vaccines save millions of lives every year already. You beg to differ? Then put up or shut up.

Du har ställt frågan om spädbarnsdödligheten minskar eller ökar vid vaccinering. När du tagit bort alla andra variabler som påverkar resultatet som svältande barn och mätta barn exempelvis, så kommer du fram till att spädbarnsdödligheten minskar vid vaccinering. Den vinsten har man alltså gjort vid vaccinering, men du gör ett fel, du drar slutsatsen genom detta resultat, att vaccin ger bättre hälsa. Du har inget belägg för det i ditt resultat. Det enda du fått veta är att spädbarnsdödligheten minskar vi vaccinering. Om du går vidare och tittar på hälsan hos befolkningen, kan du se att i de rika länderna har missfallen ökat med 58 % de senaste 10 åren. Neurologiska skador har ökat dramatiskt sedan mitten på 1990-talet. Allt fler unga får senil demens i unga år t o m i 20 års ålder och cancern har ökat lika dramatiskt den sedan 1990-talet. Du borde nu ställa dig frågan Varför? Varför har ohälsan ökat i de rika länderna som har god tillgång till näring, rent vatten, bra liv och vaccin. Även om man inte dör som spädbarn blir man sjuk som ung och vuxen. Det finns tre stora faktorer som ökat i vår livsmiljö, vaccinering, hög artificiell radiofrekvent strålning, samt storskalig spridning av kemikalier med flygplan För övrigt har industriutsläppen minskat. Du får börja räkna igen på de olika faktorerna som tillkommit de senaste 20 åren.
LikeLike
Hej Solveig, trevligt att du hittat hit! Men du hade nog lite bråttom när du läste!
“Does this say that higher vaccination uptake definitely causes lower infant mortality? No – we should generally have higher standards of evidence than this. Despite controlling for a number of confounders and taking time trends into account (and more), this is not a robust causal estimate, and it may be both weaker or stronger in reality. My point is that this estimate, if anything, is at the very least vastly more methodologically credible than any of the ones I’ve seen (even published) from anti-vaxxers – and I threw this together in half an hour with easily available data.”
Vad gäller din bredare poäng – skulle du vilja se hur korrelationerna ser ut om man istället tittar på förväntad hälsosam livslängd?
Annars är jag intresserad av några referenser på dina övriga siffror!
Vänligen,
Rafael
LikeLike
Hej! så märkligt att jag missat det stycket och läste bara det sista. Men ändå, bra att jag kom in här för nu kan du kolla närmre på det jag uppgivit. Siffrorna kommer ursprungligen från Socialstyrelsen när det gäller ohälsan. När det gäller påverkan på naturmiljön har dels jag själv dokumenterat naturmiljön i min närhet, men det finns fågelinventering, samt dokumentation över skador på djur (älgskador, sjöfågeldöd) av SVA/SLU detta gäller främst södra Sverige där man spridit chemtrails sedan slutet på 1990-talet över militära områden Skåne, Blekinge, Öland samt särskilt vid Onsala Halland där det står en stark Lofarsändare.
Missfall http://www.lu.se/article/kraftig-okning-av-kvinnor-med-upprepade-missfall
Utmattningssyndrom, Trötthetssyndrom, (elöverkänslighet döljs ofta i dessa grupper), vilket man tiger ihjäl. Att Elöverkänslighet ökar framkommer i en redovisning Örebro Landsting https://solveig21miljoblogg.files.wordpress.com/2016/02/2010-2011-c3b6rebro-landsting-forskningsstrategi-elc3b6verkc3a4nslighet-utmattningssyndrom.pdf
Neuropsykiatriska sjukdomar som ADHD, asperger, borderline har ökat . Märkliga diagnoser. Under åren har det kommit flera rapporter. Intressant är att i Värmland hade ADHD- diagnoserna ökat med 700 % på några år- Här har du underlag för att får en bild över ökningen https://solveig21miljoblogg.wordpress.com/?s=ADHD&submit=S%C3%B6k
Fåglar är främst tättingar som minskat. I denna film pekar jag på vad som minskat i min närhet . fåglar, bi , getingar humlor. https://www.youtube.com/watch?v=jC59e8ZvMcM
Man ser i svensk fågeltaxering tiden 1975-2016 tydlig minskning. OBS olika skalor har inte själv haft tid att gå igenom, men det stämmer att många fåglar har minskat. Om du kommer hit i din undersökning kan du kontakta mig så hjälper jag dig att plocka ut de viktigaste fågelarterna http://www.fageltaxering.lu.se/resultat/trender/allatrendertillsammans#Trippel8
Sjukdomsläget på vilda djur http://www.sva.se/globalassets/redesign2011/pdf/om_sva/publikationer/vilda-djur/sjukdomslaget_vilt_2009.pdf
Sedan finns det en intressant fråga till, att medeltemperaturen ökar dramatiskt på 1990-talet när man bygger ut de digitala sändarsystemen GSM, 3G, 4G kolla detta. https://solveig21miljoblogg.wordpress.com/2014/08/12/den-hoga-artificiella-mikrovagsstralningen-ar-orsaken-till-uppvarmningen-troligen/
Här fick du något att sätta tänderna i, hoppas du kan ta dig ann. När det gäller chemtrailsspridning har jag dokumenterat det över mina hemtrakter vilket också bevisas med NASA satellitbilder som du ser i min film. Men hur bena ut vad som är orsaken är kanske inte lätt. är det strålning eller chemtrails eller synergistiska effekter, det man vet är att chemtrailsspridningen är värst här nere i södra Sverige där också älgdöden är mest utbredd. När det gäller bi och getingar går har jag sett att de dör en långsam död som tar flera dagar. Man kan också visa att allt detta negativa sker sedan 1990-talet och i rasande fart. Så uppfattar man det.
Hls solveig
LikeLike